Main Body
7 Palpation
Palpation is the technique of using your hands/fingers to assess the client based on your sensation of touch. It provides the opportunity to use your sense of touch to assess the body and further examine cues that were identified during inspection.
As you prepare to touch the client, it is important that you:
- Ask permission to touch. Touch can sometimes be misinterpreted, so it is essential to be purposeful with each movement and explain what you are doing.
- Consider the warmth of your hands. Cold hands can be uncomfortable for the client. Do not blow on your hands to warm them up as this will transfer germs from your mouth to your hands. Instead, rub your hands together to create heat.
- Avoid unless indicated. The jerk-like movement can be difficult to anticipate for the client. When touching the client, use firm pressure unless otherwise indicated. Light pressure can be ticklish. In this case, sometimes incorporating the client’s hands, where possible, into your palpation technique to reduce tickling.
Palpation provides useful information to assess and evaluate findings related to temperature, texture, moisture, thickness, swelling, elasticity, contour, lumps/masses/deformities, consistency/density, organ location and size, vibration, , , and presence of pain. See Table 1.1 for specifics of how to conduct palpation based on what you are attempting to assess.
Clinical Tip
Always compare the right side and the left side of the body when palpating, because the best standard of comparison is the client’s own anatomy. The presence of a bilateral versus a unilateral finding is of clinical significance. For example, the left ankle should be symmetrical with the right ankle. The presence of edema in one ankle versus both ankles is meaningful for making judgements about the underlying pathology.
Table 1.1: Palpation techniques
|
Technique and rationale |
Consideration |
|
The dorsal aspect of your hand has thin skin relative to the rest of your hand and is therefore more sensitive to temperature. See Figure 1.8. |
Temperature refers to the degree of heat or cold an object holds. Use the dorsal surface of your own hands (i.e., the back of the hands), to assess the temperature of a surface (e.g., skin). For example, findings may include “warm skin temperature on arms, equal bilaterally.” |
|
Your fingertips are densely innervated and therefore sensitive to tactile discrimination. Recall your thumb has a pulse and therefore is not ideal for assessing pulsatility (e.g., pulses) of the client. |
Texture refers to the smoothness or roughness of a surface. For example, findings may include “smooth skin on anterior and posterior aspects of legs.” |
|
Thickness refers to how thin or thick an object is. For example, the palmar aspects (inside) of the hands and the plantar surface (bottoms) of the feet tend to have thicker skin than the rest of the body. |
|
|
Moisture refers to the amount of wetness/liquid on a surface. Is the skin dry or moist? For example, perspiration can be a normal finding in certain situations such as in a warm environment or after exercise. It can also be an abnormal finding at rest or when it is excessive, for example “ on face, arms and legs, bilaterally.” |
|
|
Swelling and masses are often assessed using your fingertips. You can also use a grasping motion with the fingertips and thumb, particularly when you are assessing the size and density of a mass. For example, some findings may include “round mass two centimetres by two centimetres midline and superior to umbilicus.” |
|
|
Pain/tenderness is best assessed while palpating with your fingertips in which your hand and wrist are kept parallel to the body so that the action does not involve poking or jabbing the client with your fingertips. Always assess a painful area last. |
|
|
The fingertips are often used to assess the various glands of the body and the organ location, size, and density, but the specific technique often depends on the organ and gland that you are assessing. For example, the fingertips can be used to assess the thyroid, lymph nodes, liver, spleen, kidney, intestines, stomach, and bladder. Findings may include “soft abdomen in all four quadrants.” |
|
|
Pulsatility refers to pulsations associated with the cardiovascular system. Most commonly, this involves placing the pads of your three fingers (starting with the index finger) over a location to assess a client’s pulse (e.g., the radial pulse or carotid pulse). You can also assess the apical impulse using the pad of your index finger. This will be discussed in more detail when you learn about the cardiac system. |
|
|
One type of crepitus is when air becomes trapped in the subcutaneous tissues of the chest/neck area; this is called subcutaneous crepitus. To palpate this crepitus, place your fingers over the chest and palpate in various areas. This will be discussed in more detail when you learn about the respiratory system. |
|
|
Cupping of hand or grasping with fingers and thumbs will allow you to gain coverage of an anatomical area while feeling for abnormalities. |
Bones and muscles (and associated deformities) as well as the trachea and testicles are often assessed using a gentle grasping motion of the fingers and thumbs. |
|
Another type of crepitation is an abnormal grating or crunching sound or sensation felt and heard over joints at the location where bones meet. It occurs when the articular surface of bones grinds together. It is different than the sounds that are made when a person cracks their fingers or joints (which are caused by the slipping of tendons/ligaments over bony surfaces). Listen and place your hand on (i.e., cup your hand over) the joint, or grasp the joint with your fingers and thumb, while asking the client to move their joints through a range of motion. This will be discussed in more detail when you learn about the musculoskeletal system. |
|
|
The metacarpophalangeal joints (base of fingers on the palmar surface) (Figure 1.9) or ulnar surface of hands/fingers (Figure 1.10) are the most sensitive to movement discrimination (vibration and pulsatility). |
Vibration is a subtle oscillating movement that resembles a quivering or shaking motion. It may be comparable to the sensation of an off-balanced washing machine, standing on a platform when the train is entering, or the sensation from a mild earthquake. Vibrations may be felt over the lungs, termed tactile fremitus; this will be discussed in more detail when you learn about the respiratory system. |
|
Pulsatility, also referred to as abnormal pulsations felt over the heart, can be assessed with the ulnar surface of your hands or the palmar surface of your metacarpophalangeal joints. These abnormal pulsations are referred to as “thrills” and will be discussed in more detail when you learn about the cardiovascular system. For example, findings may include “a thrill was palpated over second intercostal space left sternal border.” |
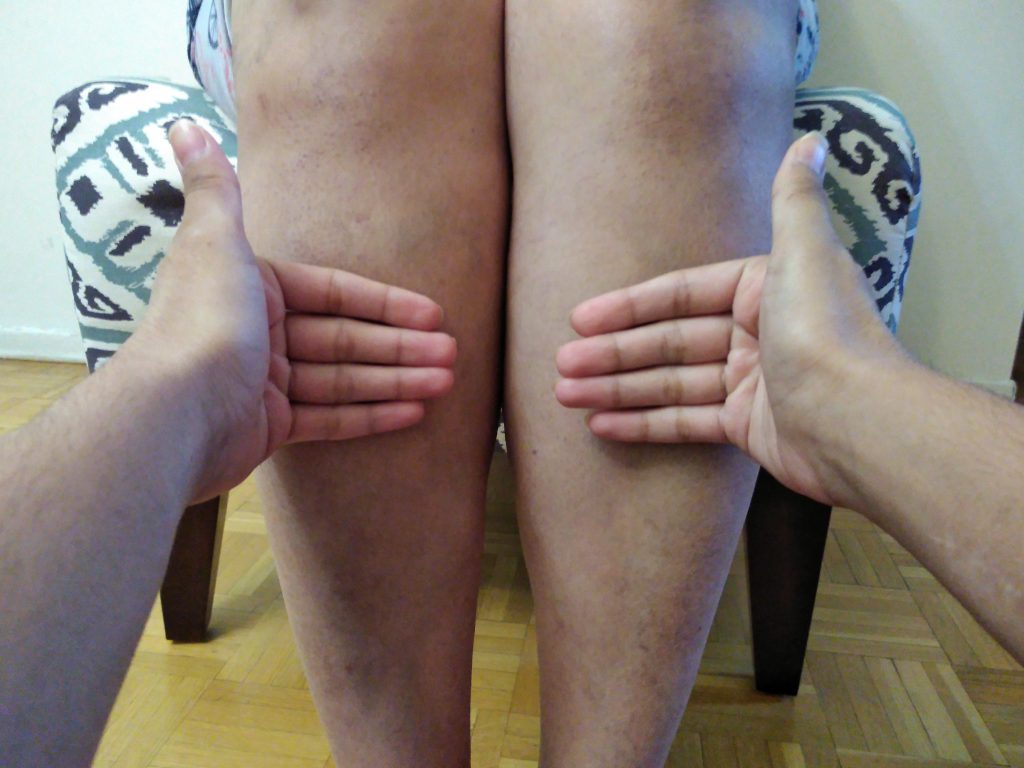
Figure 1.8: Palpating for temperature with dorsa of hands
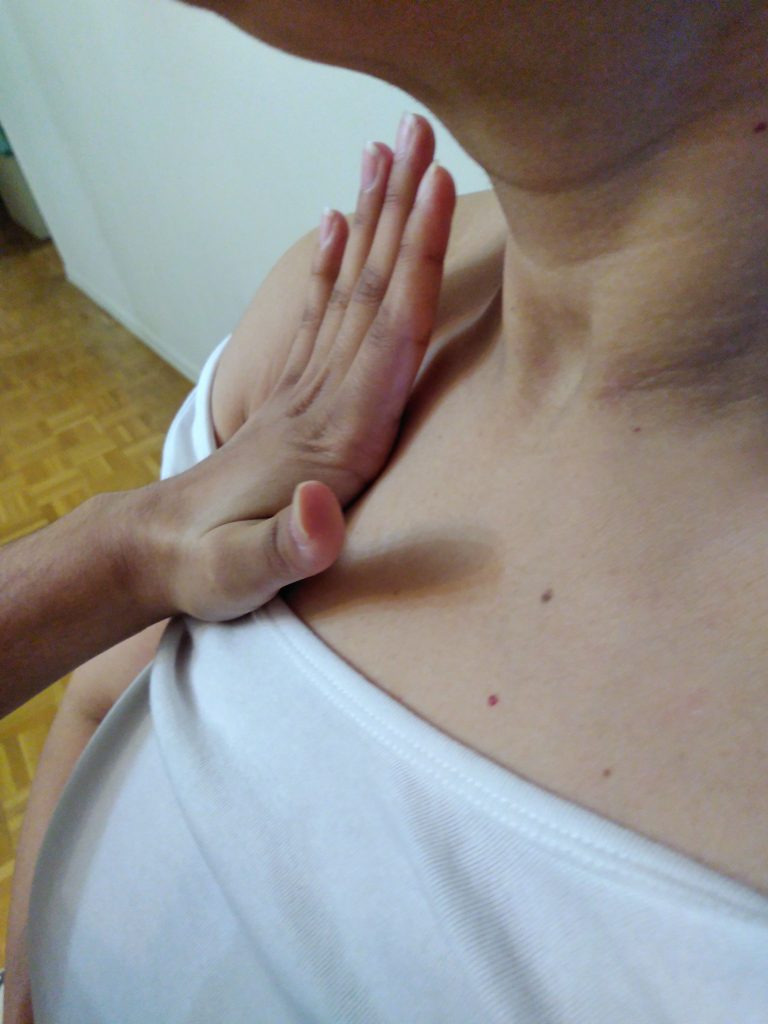
Figure 1.9: Palpating with metacarpophalangeal joints
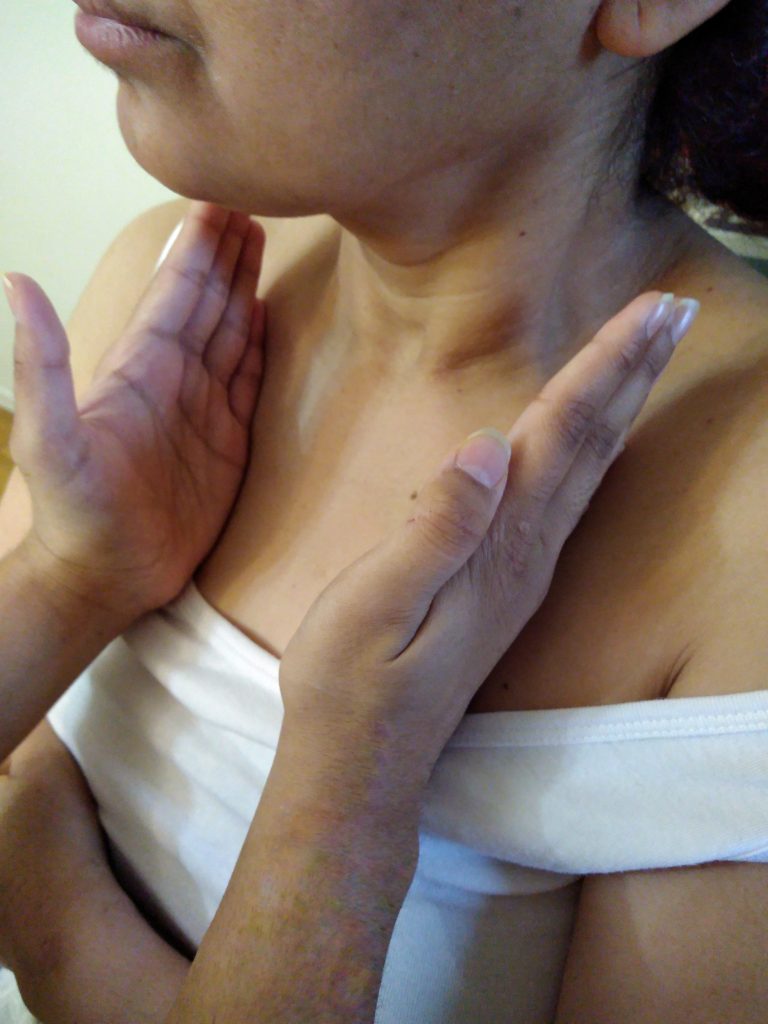
Figure 1.10: Palpating with ulnar surfaces
Voices of Experience
Distinguishing normal and abnormal findings comes with practice. It helps to familiarize yourself with common anatomy. Lab time is a unique opportunity to practice your skills and get a feel for human anatomy.
Palpation is not just an assessment technique, it is a means of communicating with your patient through touch. Consider what message you are trying to convey through touch. With young children, try to incorporate play and involve the care partner when possible. You can incorporate a child’s toy or teddy bear into the assessment. If a child is ticklish, you can engage them by placing their hand on top of yours and ask them to move your hand to various positions to palpate.
For all clients – children, adolescents, and adults – assess their readiness to touch. For example, you may begin by palpating non-invasive areas such as the hands first, and always explain what you will be doing. It is important to observe facial expression as an indicator of how the client is responding and also whether they are in pain.
Quick, short taps.
The quality of pulsations, such as the pulse.
The abnormal grating or crunching sound over moving joints.
Excessive perspiration.

